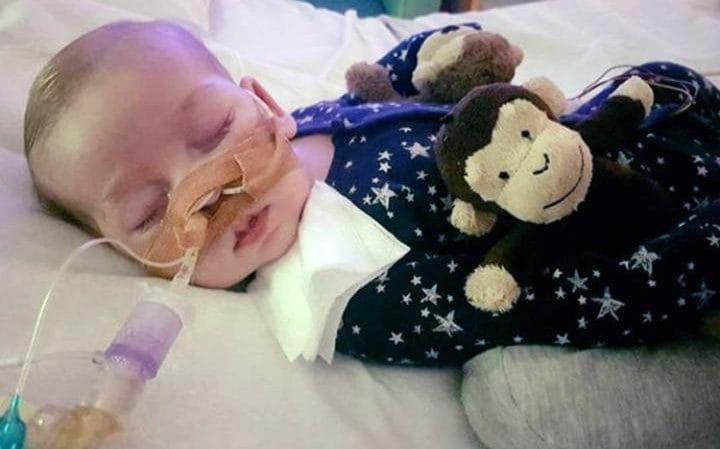
Charlie Gard
Charlie Gard, the terminally ill baby at the center of a five-month long legal battle, is front-page news everywhere this week, but not for the reasons we’d like.
There will be no further treatment for Charlie, experimental or otherwise, as his parents have elected to discontinue life-support measures and watch their infant son die, just days before his first birthday.
Charlie suffers from a rare genetic condition known as encephalomyopathic mitochondrial DNA depletion syndrome (MDDS). Children with MDDS very rarely survive to see adolescence; most die before their second birthday. In Charlie’s case, the condition has caused severe, irreparable brain damage. He cannot see, hear, swallow, or cry.
Charlie was a perfectly normal appearing newborn, but his condition began to deteriorate quickly. He has spent his life in an intensive care unit. While other babies are rolling over and learning to crawl, Charlie is bound to a bed, intubated; a machine is doing the work of breathing for him.
Physicians at Great Ormond Street Hospital (GOSH), the facility treating Charlie, assessed him earlier this year and determined that his brain damage was too significant to be treated. Charlie’s parents, Chris Gard and Connie Yates, asked that GOSH allow Charlie to be released to undergo an experimental treatment in the US. But given his advanced neurological deterioration, combined with the unlikely success of the treatment, the hospital declined their request, and thus began the five-month legal battle that would culminate this week in the decision to discontinue support.
Parents all over the world mourn with Charlie’s parents today.
The cost of the treatment was more than sufficiently covered by fundraising efforts. Whether or not the treatment could have been successful, however, is a question we are unable to answer.
But is it a question we need to answer?
♦♦♦
In the wee hours of a cold winter morning, an obsolete Nokia mobile phone rings beside my bed. It’s Shirley at the answering service relaying a desperate message from the 38-year-old mother of an infant in my care. He is not breathing. She does not know what to do. I am 15 minutes from her home, which is 15 minutes too far.
A hospice nurse on call sleeps lightly and near her car keys, knowing a grave concern could arise at any moment. A woman might call to report that her husband’s breathing is shallow and loud. An adult child might call to ask how to manage their mother’s pain. A parent might call, panicking as they watch the clock run out on their terminally ill baby.
I sleep fully clothed because it’s easier than getting dressed in the dark. My belly has begun to swell over my feet, a tiny, healthy baby wiggles and twists inside me. I fumble through the dark and out my door, locking the deadbolt behind me. An oversized sweater and leggings hide the evidence of my fifth pregnancy, something I do not want this mother to see.
It is winter. Winter in Central California is more foggy than cold — the air is thick and heavy and sticks to your windows. Fog is just the kind of weather that feels appropriate tonight; someone’s baby is dying.
Sometimes the fog burns off when the sun hits midday, but it will not burn off this afternoon. The sun will not shine for this family today.
They knew the baby was going to die before he was born.
When parents know ahead of time that their child has a terminal illness, they will often be offered the option to terminate the pregnancy. They usually do not do this.
Is the pain of watching your child die any more devastating than never seeing them alive?
Even when we know that a baby cannot live, even if their heart cannot circulate their blood, or their brain is missing but for the very base of it, even then, there is hope. When your child is dying, even as they are dying, there is hope.
When medicine delivers the worst prognosis they can imagine, hope is all a parent might have.
This mother knows her baby is dying. She has known this since she was in the early weeks of her second trimester. A blood test suggested it. An ultrasound confirmed it. Her baby will not live to see his first birthday; he may not live to see the end of his first month.
She knows this.
Her husband and other children know this. Her family knows this. The people from her church delivering casseroles and taking her other children on extended playdates know this.
Despite knowing this, he has a car seat. He has a dresser full of tiny folded shirts and pants and elephant covered sleepers with zippers that he will never wear. He has a nursery, all blue and green and serene, where he will never sleep. There is a big rocking chair in the corner. She will hold him in this chair while he dies. We know he will die.
But tonight, as I drive, eyes heavy with exhaustion, he takes his final breaths, and she tries to save him.
Hospice care isn’t a thing we do for people who are fighting to live. Hospice care is a thing we do when we know that people are going to die, when we want to give them the chance to do that on their own terms. Hospice is not meant to save; it is meant to comfort.
But on this foggy night, the DNR is forgotten, an ambulance is called, a mother tries frantically to save her baby's life.
It does not matter that he cannot, that he will not, live.
All that matters in the last gasping moments is that this is her child. This is a child she wanted desperately. A child she waited for. A child she prayed for a miracle for.
What do the courts say about Charlie Gard? What could an experimental treatment offer for Charlie?
What does it matter?
In the matter of your child’s life, wouldn’t you try anything? Would you fly him around the globe for an experimental treatment?
Would you give him your kidney or liver or lung?
Would you perform CPR as you watched him slip from your arms out of this world? Even if you signed a Do Not Resuscitate order, would you remember that order that sits in a file somewhere in your kitchen buried under piles of cards from people who can’t empathize, people who will never hold their dying child?
Would you care?
Charlie's case has raised some intense questions of ethics. Should he have received experimental care despite his grave prognosis? And at what point does treatment go from caring to cruel? In medicine, these will always be the most difficult questions to answer, the most complicated situations to navigate.
In life though, it’s very simple: We will always choose to hope for our babies.







